2026 Municipal Alliance Brochure

March Is Problem Gambling Awareness Month!
Neptune Alliance, March 2025 Prevention Article
Each March, National Problem Gambling Awareness Month seeks to increase public awareness of problem gambling and promote gambling prevention, treatment, and recovery services. The 2025 theme, “Seeking Understanding,” highlights how problem gambling is often overlooked as a serious mental health condition that deserves empathy and access to treatment and support resources.
The National Council on Problem Gambling estimates that 2.5 million U.S. adults have a severe gambling problem, with another 5 to 8 million experiencing mild or moderate issues with gambling. While most adults who gamble do so responsibly, the effects of problem gambling can be emotionally and financially devastating for individuals and families (https://www.ncpgambling.org/help-treatment/faqs-what-is-problem-gambling/).
Problem gambling continues to rise at alarming rates due to online casino and sports betting apps, which appeal to younger gamblers. These apps allow users to place bets discreetly and 24/7, whether at home, at work, socializing, or on the go.
Statistica anticipates that by 2029, online gambling will grow to a $40-billion industry in the U.S. The online gambling market reached over $19.5 billion in 2023. In 2024, Statistica research identified bet365 as the most popular sports gambling platform for adults ages 21 to 34; DraftKings and FanDuel were preferred by those 45 years and older (https://statstica.com/forecasts/1318601/online-gambling-market-size-us).
Youth face a higher risk than adults for developing a gambling problem, and individuals who start gambling at a young age are more likely to develop an addiction to gambling throughout their lifetime, just like with alcohol and substance use disorders and early onset of use.
Signs of problem gambling include…
- Lying about your gambling
- Using gambling as an escape from daily living and responsibilities
- Being unable to control your gambling or betting
- Chasing losses
- Racking up debt or stealing to fund your gambling habits
- Risking relationships or opportunities
If you or someone you care about needs help with a gambling issue, here are options for support:
- National Problem Gambling Helpline: 800-GAMBLER (call, text, and chat services, 24/7, 365 days a year) or https://www.ncpgambling.org
- Gamblers Anonymous: https://gamblersanonymous.org (virtual and in-person support groups)
- National Council on Compulsive Gambling: https://www.ncpgambling.org/ncpg/
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Substance Use Disorder
Social Media Parent Guide
Please CLICK HERE to view
Guardian Prevention Resource
Please CLICK HERE to view

April Is Alcohol Awareness Month
Neptune Alliance, April 2024 Prevention Article
During April’s Alcohol Awareness Month, people of all ages—from teens through seniors—are encouraged learn more about the effects of consuming alcohol; alcohol use disorder; the negative impact alcohol misuse has on individuals, families, loved ones, and society; and support resources available for those impacted by problematic alcohol consumption.
Excessive alcohol use increases the odds of alcohol overdoses and poisonings, injuries, poor pregnancy outcomes, sexual and physical assaults, motor vehicle crashes, homicides, suicides, risk- taking without regard for consequences, dysfunctional relationships, and chronic diseases (such as mental and behavioral disorders, liver and heart disease, and cancer).
Consuming alcohol under the legal age of 21 can interfere with normal brain development and increase the chance of alcohol use disorder across a lifetime, in addition to the risks mentioned above.
Despite these negative outcomes associated with alcohol misuse, alcohol use disorder is one of the mental disorders with the lowest treatment rates due to a lack of awareness, denial, stigma, shame, low risk perception, social normalization, and limited access to support resources.
How prevalent is alcohol misuse? Approximately 3 million people die each year of harmful alcohol use worldwide (World Health Organization, 2022). Approximately 16 million Americans were heavy alcohol users and 14.5 million Americans had an alcohol use disorder, according to the 2019 National Survey on Drug Use and Health. The same survey also shared that about 7 million adolescents ages 12 to 20 reported current alcohol use, despite 21 being the legal age for alcohol consumption.
If you or someone you love or know is struggling with alcohol misuse or alcohol use disorder, here are some of the support resources available:
Alcoholics Anonymous, or AA, (www.aa.org) is an international fellowship of people of all ages who have had a drinking problem. There are local AA chapters who meet in communities around the world. The AA website noted above provides information on where to find a meeting in your community.
Through using an online, anonymous screening tool at www.alcoholscreening.org, individuals can assess their own drinking patterns to determine if their alcohol use is harmful or hazardous. There are also strategies suggested for lowering drinking-related risks and getting help.
The Substance Abuse and Mental Health Services Administration (SAMHSA) offers a free, 24/7, and confidential national helpline at 800-662-4357 for individuals and families impacted by alcohol misuse or abuse, or other substance use and mental health disorders. Support resource referrals and information services are available to English and Spanish speakers through this helpline.
The National Institute on Alcohol Abuse and Alcoholism (NIAAA) (www.niaaa.nih.gov/) provides information on alcohol consumption and actual serving sizes across different types of alcohol, warning signs of a drinking problem, and individual and group support services.
Alcohol misuse on college campuses brings consequences that can forever change the lives of students, parents, family, classmates, and friends. Some college binge-drinking and underage drinking tragedies have made news headlines, but many do not; however, all of the devastation caused by problem drinking is preventable through education, proper decision-making, and regard for potential outcomes. Visit the website College Drinking: Changing the Culture (www.collegeddrinkingprevention.org) for information on college drinking statistics, school-specific alcohol policies, alcohol myths, alcohol consumption calculators, and interactive activities about how alcohol affects nearly every organ in the body.
Parents can learn more about underage drinking and prevention strategies by reading “Underage Drinking and Teen Alcohol Use” at www.helpguide.org/articles/addictions/underage-drinking.htm.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
The Neptune Township Municipal Alliance to Prevent Alcoholism and Drug Abuse would like to extend a huge thank you to all who helped make the sixteenth annual Cops vs. Kids basketball game on March 12 such a success! The prevention message was clear; the game was fun, and the Cops and Kids enjoyed some friendly competition.
It was a great event—from pre-event sponsorship to the last basket. The Cops continued their winning streak with an 61-51 victory. Spectators attempted foul shots at half time, while wearing Fatal Vision Goggles, simulating what it’s like to be impaired by drugs or alcohol. Not many shots even came close!
Dozens of youth in attendance won prizes, and the grand prize winner of the cruiser bicycle was Kailynn Lavern!
The Kids’ team (coached by Matt Gorman) included: David Boone, Lana Ellington, Daren Fonrose, Robens Jordonne, Aaron Lawson, Julian Lemus, Daaron Lynch, Mike MacLennan, Stephen McQuay,
Daniel Merritt, Jayden Myrthil, Majiah Quarles, David Ramirez, Jayvion Rogers, Nick Sapp, Phil Singleton, Donovan Steverson, Cameron Stukes, Alex Velasquez, Kimani Wallace, and Tyshawn Wilder.
The Cops’ team (coached by Jim MacConchie) included: Lt. Kaan Williams, Josh James, Jaheem Woods, Marcus Alston, Sgt. Mysonn Ledet, Lt. Robert Baldwin, Nick Krimin, James Weinberg, Robert Newman, Briant Nixon, Scott Gomez, MiJaut Berry, Matt McDonough, Tressa Yurman, Javaugh Rogers, Deputy Chief Mike McGhee, and Chief Anthony Gualario.
Special volunteer thanks also to: Catherine Crelin for coordinating the Kids’ team and school logistics; Mark Clark for refereeing; Ken Maher for scoring & timing; Del for announcing, Lana Ellington for singing the Star-Spangled Banner, Neptune Cheerleaders, Neptune ROTC, the players, coaches, Neptune Board of Education; Patty Sneddon for refreshment help, and Prevention First / Prevention Coalition of Monmouth County for hosting a table with prevention giveaways at the event.
Thanks to all of our event sponsors, including: Neptune Township Police PBA #74, Neptune Twp FOP #19, McDonalds Rte 33 & 66, Jersey Mike’s Subs, Theo’s Demolition & Construction Clean-Up, Impact Auto Body, Bruno’s Italian Deli, MJ’s Pizza Bar & Grill, Allied Fire & Safety, Uni-Serv, Inc., Target, Neptune Board of Education & High School, the Neptune Municipal Alliance to Prevent Alcoholism and Drug Abuse, Midtown Urban Renaissance Corporation (MURC), and the Neptune Recreation Department. Funding for this event is also provided through the Governor’s Council on Alcohol & Drug Abuse.
Thanks to everyone who supported the game, and in turn, helps us spread our prevention message to the community. Be sure to look for our next Cops vs. Kids fundraiser, as I heard more than one, “Wait till next time!”
Sincerely,
Dawn Thompson, Recreation Director & Coordinator, Municipal Alliance to Prevent Alcoholism and Drug Abuse
February 26th - March 3rd is National Eating Disorders Awareness Week
February 2024 Neptune Alliance Prevention Article
National Eating Disorders Awareness Week begins annually the last Monday of February; this year, it will be observed February 26th through March 3rd.
During National Eating Disorders Awareness Week and through its work year-round, NEDA aims to…
- spotlight eating disorders
- give hope to those affected by eating disorders
- improve understanding of and education on eating disorders
- alert the public to the disease’s dangers
- provide information on treatment options and recovery programs
- highlight the need for early detection and intervention to save lives
- serve as a catalyst for prevention, cures, and access to quality care. According to NEDA…
- Eating disorders have the highest mortality rate of any mental disorder
- 20 million women and 10 million men suffer from a clinically significant eating disorder at one point in their lives
- Eating disorders can surface as anorexia nervosa, bulimia nervosa, binge eating disorder, or an “other-than-specified” eating disorder
- Over 50% of teenage girls and nearly 33% of teenage boys use unhealthy means to control their weight such as skipping meals, smoking, fasting, vomiting, and taking laxatives.
Signs of an eating disorder include…
- drastic weight loss
- fixation on counting calories
- focus on body weight and shape
- excessive exercise
- shame or guilt about eating
- binge eating and purging
- unusual eating rituals
- eating alone
People of all ages, genders, and body types can develop eating disorders, which can be challenging to diagnose, particularly in children. Early diagnosis and interventions are key to saving lives when it comes to eating disorders.
With today’s youth using social media for often several hours a day and comparing themselves to altered and unrealistic celebrity and influencer images, eating disorders and difficulties with body image in children and teens are on the rise and starting at younger ages.
For more information on NEDA and National Eating Disorders Awareness Week, visit www.nedawareness.org.
NEDA’s website has an online screening tool for eating disorders, recovery tips, and personal stories of hope from people in recovery. It also provides information on various eating disorders, help resources for those affected by an eating disorder and their loved ones, and information on how to get involved in the fight against eating disorders.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Xylazine Fact Sheet
Please CLICK HERE to view
E-Cigarettes and Vape Disposal
The Monmouth County Reclamation Center at 6000 Asbury Ave, Tinton Falls, NJ 07753 is now accepting used and unwanted e-cigarette cartridges at their facility! Residents and school officials are welcome to drop off their spent e-cigarette devices to be disposed of in a safe and environmentally friendly way without having to disassemble the devices on their own. The Reclamation Center hours are Monday-Friday 7:00 am - 3:30 p.m. and Saturday 7:00 am - 12:00 pm.
New Jersey Prevention Network
The Marijuana Municipal Toolkit - Cannabis Legalization and Local Policy: A Public Health Approach can be downloaded free here: https://www.njpreventionhub.org/policy-toolkits


When the Holidays Aren’t Happy: Coping Strategies for the Holiday Blues
Neptune Alliance, November 2023 Prevention Article
The pressure to experience the perfect, magical, and happy holiday season can cause stress and sadness for some. Reasons you or someone you know may struggle with the holiday blues include…
trauma, grief, or unpleasant memories
the loss of a loved one
difficult family relationships or the end of a relationship
anxiety or depression
loneliness or social isolation
pressure to participate in social gatherings and festivities
financial stress
the anticipation of awkward or uncomfortable topics of conversation
unrealistic expectations to have the “perfect” holiday season
a lack of holiday spirit
During the holidays, it is also important to look out for and be respectful of those struggling with mental health and/or substance use disorders. According to the National Alliance on Mental Illness (NAMI), 64% of individuals living with a mental illness said they felt worse around the holidays.
This time of year, try to be mindful that the holiday season may not be celebratory for everyone, including you. Creating realistic holiday expectations, knowing your trigger stress points, and preparing ahead with coping strategies can provide a sense of control, relief, and calm.
For helpful strategies to lift your holiday spirits, alleviate anxiety and depression, and cope with sadness during a time when the rest of the world appears to be happy, read these articles, or share them with someone you think may struggle this time of year:
“Seven Ways to Cope with Thanksgiving Blues,” https://www.psychologytoday.com/us/blog/two-takes-depression/202211/7-ways- cope-thanksgiving-blues (Psychology Today)
“Hate the Holidays? Here Are 8 Ways to Cope and Find Joy This Year,” https://www.mcleanhospital.org/essential/mcleans-guide-managing-mental- health-around-holidays (PsychCentral)
“Spending the Holidays Alone? 8 Coping Strategies,” https://psychcentral.com/health/spending-holidays-alone-coping-tips (PsychCentral)
“Guide to Managing Mental Health Around the Holidays,” https://www.mcleanhospital.org/essential/mcleans-guide-managing-mental- health-around-holidays (McLean Hospital)
“Holiday Grief: How to Cope with Loss During a Joyous Time,” https://www.verywellmind.com/holiday-grief-how-to-cope-with-loss-during-a- joyous-time-6503042 (Verywell Mind).
No matter the time of year, call 9-1-1 if you or someone you know is facing an immediate mental health or substance use crisis or may be of harm to themselves or others.
The 988 Suicide and Crisis Lifeline is available 24/7 by calling or texting 9-8-8 (https://988lifeline.org/). The Crisis Text Line also provides 24/7 support for an emotional crisis by texting “HOME” to 741741 (https://www.crisistextline.org).
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse

Neptune Township joined other municipalities in Monmouth County in supporting International Overdose Awareness Day with a purple flag display!
Overdose Awareness Day remembers loved ones lost to overdoses and supports ending the stigma of drug-related deaths. The purple flags placed in front of the Neptune Township Municipal Building this week represent the Monmouth County residents whose lives were lost to overdoses in 2023. The display also recognizes the countless more residents who have been forever affected by overdose deaths.
Overdose Awareness Day is August 31, and the flags will be on display until early September.
Taking part in the Neptune recognition were: Neptune Deputy Mayor Tassie York; Prevention First, a Division of Preferred Behavioral Health; Monmouth County Municipal Alliance Coordinator Billy Horbatt; Neptune Township Police; members of the Prevention Coalition of Monmouth County; the NJ Counter Drug Task Force; Seacrest Recovery Center; the Neptune Township Municipal Alliance to Prevent Substance Misuse; Neptune Recreation; and several Neptune Township employees.

Mental Health & Substance Use Support Services
Neptune Alliance, August 2023 Prevention Article
Mental health and substance use disorders affect millions of Americans, many of whom do not seek or receive assistance due to stigma, fear of judgment, or a lack of access to resources.
In the United States…
- 1 in 4 adults and 1 in 6 youth experience a diagnosable mental disorder in any given year (National Institute of Mental Health)
- 42% of high school students experienced persistent feelings of sadness or hopelessness during the past year that stopped them from doing their usual activities (CDC’s 2021 Youth Risk Behavior Survey)
- 48 million adults experience an anxiety disorder (National Alliance on Mental Illness)
- Less than 50% of adults receive the mental health services and treatment they need (Mental Health America)
- Almost 110,000 drug overdose deaths per year occurred in both 2021 and 2022 (CDC)
- 46.3 million people aged 12 or older met DSM-5 substance use disorder criteria in the past year; 29.5 million met alcohol use disorder criteria and 24 million met drug use disorder criteria (SAMSHA’s 2021 National Survey on Drug Use and Health)
Should you, a loved one, or someone you know experience a mental health or substance use disorder, here are crisis helplines and community support resources that can help:
- Always call 911 for an immediate crisis or dangerous or life-threatening situation!
- 988 Suicide and Crisis Lifeline: 24/7, free, confidential emotional support in English and Spanish from a national network of crisis centers; for anyone experiencing a suicidal crisis or emotional distress; call or text 988, or use the online chat; https://988lifeline.org/
- Crisis Text Line: 24/7, free, confidential support in English and Spanish from trained volunteer crisis counselors; for anyone experiencing a crisis; text “HOME” to 741741, use the online chat, or message them on WhatsApp; https://www.crisistextline.org/
- 2ndFLOOR Youth Helpline: 24/7, free, confidential support in English and Spanish from trained volunteers; offers guidance to anyone in NJ ages 10 to 24 when facing issues or problems emotionally, socially, at school, or at home; call or text 888-222-2228; https://www.2ndfloor.org/
- NJ Poison Control hotline: 24/7, free, confidential support in English, Spanish, and other languages from specially-trained health care professionals; offers anyone assistance with questions and concerns for poisonings, medication and food safety, household cleaning products, carbon monoxide, and drug overdoses; call 800-222-1222; https://www.njpies.org/
- Monmouth ResourceNet: provides a wide range of information about support, resources, and services for Monmouth County residents, including behavioral/ mental health, crisis/safety, and medical support services; https://www.monmouthresourcenet.org/
- Monmouth County Children and Youth Behavioral Health Resource Guide: provides access to locally organized and integrated systems of youth behavioral health and support services for Monmouth County community members; https://www.co.monmouth.nj.us/documents/41/Child-Behavioral-Health-Reference-Guide_2022-23_Web_Email.pdf
- Monmouth County Behavioral Health Resource Guide: provides Monmouth County community members with access to locally organized and integrated systems of support services to prevent, intervene, treat and recover from behavioral health challenges; https://www.co.monmouth.nj.us/documents/41/Behavioral-Health-Reference-Guide-Section_for-county-web_2022.pdf
- Naloxone365: State of NJ’s free naloxone distribution program for anyone ages 14 and up; for a list of participating pharmacies in Neptune and nearby towns, visit https://data.nj.gov/Human-Services/Naloxone365-NJ-Free-Naloxone-at-Pharmacies-Program/nfsa-3664/data.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Kratom Is Readily Available, Yet a Drug of Concern for the DEA
Neptune Alliance, July 2023 Prevention Article
Despite being an herbal substance easily accessible to youth, the psychotropic supplement kratom comes with the potential for harm and addiction, making it a “drug of concern” for the Drug Enforcement Administration (DEA).
Kratom is legally sold over-the-counter in many local head shops, vape stores, convenience stores, gas stations, and even health and vitamin stores, as well as online. People use the supplement as a sedative, pain reliever, and stimulant. It is also taken by some to prevent opioid withdrawal.
Available in pill, capsule, extract, and leaf forms, kratom can produce both opioid- and stimulant-like effects, with its active ingredient varying. In addition, the unregulated products may contain contaminants such as pesticides, mold, heavy metals, and salmonella.
U.S. poison control centers received 1,800 reports involving use of kratom from 2011 to 2017, including deaths. In 2011, there were 13 reported exposures; in 2017, the number jumped to 682, going from one call per month to two calls per day. About half of these had serious negative outcomes, such as seizures and high blood pressure, yet kratom’s availability and consumption rates continue to rise.
Learn more about kratom on the websites below, then share the information with youth you know to alert them to the dangers kratom poses. Just because a substance is legal and readily available doesn’t mean it is safe, especially when it comes to youth. The brain continues to develop until at least age 25, making it more susceptible to long-term consequences and addiction.
Signs of a kratom overdose vary and can include shallow breathing, a weak pulse, nausea, vomiting, drowsiness, confusion, agitation, hypertension, and a fast heart rate. It can also lead to unconsciousness and a coma.
- “Drug Fact Sheet: Kratom” on the DEA’s Just Think Twice website: https://www.justthinktwice.gov/sites/default/files/2022-11/Kratom%202022%20Drug%20Fact%20Sheet_0.pdf
- “Kratom: Unsafe and Ineffective” by the Mayo Clinic: https://www.mayoclinic.org/healthy-lifestyle/consumer-health/in-depth/kratom/art-20402171
- “Kratom Overdoses Are on the Rise. Why They’re Hard to Spot” on Healthline’s website: https://www.healthline.com/health-news/how-to-spot-a-kratom-overdose.
(The above websites are also referenced in the article.)
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
June 2023 Neptune Alliance Prevention Article
Marijuana Edibles Poisonings Rise Alongside Legalization
With the legalization of adult-use recreational marijuana (or cannabis) in New Jersey and 21 other states, concern is growing over the rise in marijuana edibles poisonings that parallels the increase in marijuana availability.
From 2017 to 2021, there were over 7,000 cases of children under 6 years old ingesting marijuana edibles in the U.S.–a 1,375% increase from 200 cases in 2017 to over 3,000 in 2021. A quarter of these reported cases required hospitalization.
Between 2005 and 2019, the increase in marijuana-related emergency room visits in the U.S. jumped 1808%, from 366 in 2005 to 12,167 in 2019.
THC potency levels are also climbing across the legal and black markets. THC is the psychoactive ingredient in marijuana that causes the high and impairs judgment, decision-making, perception, vision, and coordination. The average THC level was 3% to 5% a few decades ago; today, the average THC level is 55%, with 100% THC potencies available in concentrated, synthesized forms. New Jersey and most other states allowing recreational cannabis use do not have a THC potency cap included in their laws.
This is coupled with the fact that the 2018 Farm Bill federally legalized hemp production, removing it from the DEA’s list of controlled substances. When hemp’s trace amounts of THC are synthesized into products such as Delta-8, potent levels of THC become legally and readily available in stores and online to people of all ages, including youth.
The packaging and presentation of THC-containing edibles often resemble familiar, brand-name snacks, gummies, lollipops, chocolate candies, and desserts that look appealing and safe to consume in any desired quantity. Most people pay little to no attention to the THC dosage per recommended serving listed on the package, leading to unintentional consumption of high THC levels and marijuana toxicity. Young children who are smaller in size and seek sweets are particularly vulnerable to accidental THC poisoning, as are seniors due to their slower metabolism, interest in marijuana for aches and pains, and lack of information about today’s potent THC products.
When marijuana is ingested orally, it can take one to four hours to experience the peak of the high, whereas when marijuana is inhaled, the high occurs within five minutes to half an hour. With this delayed response to the THC in marijuana edibles, it is easy to keep consuming marijuana products, leading to toxic levels in the body and brain.
THC poisoning can be life-threatening, especially for children. Should you suspect someone is suffering from THC poisoning, immediately call 9-1-1. You can also call the NJ Poison Control Center at 800-222-1222.
Signs of marijuana poisoning, or cannabis toxicity, include…
- overwhelming sleepiness, beyond what’s typical at bedtime
- trouble breathing
- irregular heartbeat, chest pain
- collapse
- agitation and hyperactivity
- seizures
For more information on marijuana, go to Every Brain Matters’ educational resources at https://everybrainmatters.org/marijuana-infographics-for-education/.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Sticks and stones may break bones, but stigma kills | Opinion
by Nikki Tierney Star-Ledger Guest Columnist May. 08, 2023
Nikki Tierney is a licensed professional counselor and licensed clinical alcohol and drug counselor. She says studies have shown that using scientifically accurate language and terms that centralize the experience of people with substance use disorders is one key component to reducing stigma.
The human brain produces a response to words, which is a process known as associative activation. Certain words also produce unconscious association, known as bias.
People have deeply ingrained biases of which they are completely unaware. This implicit bias influences how people treat others, often with unintended discriminatory consequences.
Stigma is a word that comes from Latin and Greek, and originally meant a burn, tattoo, or other mark inflicted on another person to signify their disgrace. Today, stigma means labeling, stereotyping and discrimination.
In relation to substance use disorders, stigma is often connected to the cognitive distortion that people with substance use disorders have chosen their plight and are somehow less deserving of empathetic and dignified treatment than people with other chronic medical conditions.
Both the public and ironically, some professionals who treat people with substance use disorder consider the cause of substance use disorder to be a lack of willpower and a moral failing. However, these theories have been proven incorrect and harmful.
For example, Rahul Gupta, the first physician to serve as a drug czar, says stigma is a key culprit in addiction crisis.
“Right now, we use all kinds of derogatory terms for people,” Gupta said in a STAT interview. “We have, obviously, the stigma that prevents so many people from asking for help and others from providing the help. It’s both — in communities, but also in health care.”
The terms substance abuse, drug addiction, alcoholism, and addicts are not only stigmatizing and dehumanizing, but they are also inconsistent with The Diagnostic and Statistical Manual of Mental Disorders, which is authored by the American Psychiatric Association (APA.)
More specifically, the APA no longer uses the terms substance abuse and substance dependence, rather it refers to substance use disorders, which are defined as mild, moderate, or severe to indicate the level of severity, which is determined by the number of diagnostic criteria met by an individual.
In the United States, nearly 90% of people with substance use disorders and 35% of people with serious mental illness do not receive treatment.
A recent article published in Neuropsychopharmacology discusses how people with a mental illness or substance use disorder who experience stigma may begin to internalize it, leading to lower self-esteem, decreased interest in seeking help and worsening of their symptoms.
Studies have shown that using scientifically accurate language and terms that centralize the experience of people with substance use disorders is one key component to reducing stigma. Such efforts can improve how people with these conditions are treated in health care settings and in society.
The New Jersey legislature has taken a bold step to remove the stigma from the New Jersey statutes and names of government entities. More specifically, Sen. Gopal and Assemblyman Wimberly have introduced S3511 and A5096, respectively.
This legislation in accordance with science, studies, and data revises our laws and entity names using non-pejorative, non-stigmatizing, person-first language to describe substance use disorders and those affected by such disorders.
Legislative bills S3511 and A5096 represent a cost-free means for New Jersey to be a leader in the nation in creating a truly stigma-free environment for people living with mental health and/or substance use disorders.
These bills will save lives, increase the number of people receiving treatment for mental health and substance use disorders, and reduce the impact of these chronic medical conditions not only on the people who experience these disorders, but their families, loved ones, and society as a whole.
Both bills have broad bipartisan support, and the Assembly version has been reported from Committee unanimously and is awaiting a vote by the full Assembly.
Our legislature should act expeditiously to pass these bills, and Gov. Murphy should sign them immediately to end stigma in New Jersey.
Nikki Tierney, J.D., M.S. is a licensed professional counselor and licensed clinical alcohol and drug counselor. She is also in sustained remission from opioid use disorder.
May 2023 Neptune Alliance Prevention Article
Tips for Starting Conversations with Your Children About Alcohol and Drug Use
Starting conversations with your children about alcohol and drug use is never easy, but it is very necessary, as prevention starts with parents!
If parents talk to their children regularly, directly, respectfully, and honestly about alcohol and drug use, their children are more likely to respect their rules and advice and avoid many of the high-risk behaviors associated with alcohol and drug use (https://www.samhsa.gov/sites/default/files/talk-with-your-child-about-alcohol-drugs.pdf?).
Since the brain develops until at least age 25, delaying the age of first-use of any substance is critical, including nicotine, alcohol, and marijuana, as well as the misuse of prescription and over-the-counter medications and illicitly obtained drugs like opioids.
Age-appropriate conversations about alcohol and drug use should start early on and don’t have to last long. Parents should listen actively, avoid lecturing, and strike up conversations when the time is right, in a comfortable and relaxed setting, or when children ask questions.
The “Awkward Conversations” podcast series presented by the Elks Drug Awareness Program (DAP) covers a wide array of subjects to educate parents on raising kids with the tools necessary to stay safe and substance free—and to make smart decisions in general. A link to “Awkward Conversations” is provided below.
Each “Awkward Conversations” episode features expert guests who help guide parents and answer those tough questions parents may have in the ever-changing world of raising kids.
“Awkward Conversations” topics covered include:
- signs of drug use in teens
- fake pills
- setting positive examples
- preventing drug misuse among college students
- bullying and peer pressure and its consequences
- helping kids de-stress
- understanding your kids’ social media use
- do’s and don’ts when you talk about drugs
Watch podcasts from “Awkward Conversations” seasons 1 and 2 on the Elks Drug Awareness Program’s website: https://elksdap.org/resources/awkward-conversations.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Interesting article from the New York Times:
This Is What Neuroscientists and Philosophers Understand About Addiction
By Maia Szalavitz April 24, 2023
Ms. Szalavitz is a contributing Opinion writer who covers addiction and public policy.
Sign up for the Opinion Today newsletter Get expert analysis of the news and a guide to the big ideas shaping the world every weekday morning.
When I was arrested and charged with possession with intent to sell cocaine in 1986, I was addicted to both coke and heroin. Although I was facing a 15 years-to-life sentence, the first thing I did after my parents bailed me out and held a family meeting was to find and secretly inject some prescription opioids that I knew the police hadn’t confiscated.
I knew that doing this further jeopardized my life prospects and my relationships with everyone I cared about. I knew it made no sense. But I didn’t believe that I could cope in any other way. Until I finally recognized that I needed treatment and began recovery in 1988 — with the prospect of that lengthy sentence under New York’s draconian Rockefeller laws still occluding my future — I didn’t think I had any real choice.
Was my brain hijacked by drugs — or was I willfully choosing to risk it all for a few hours of selfish pleasure? What makes people continue taking drugs like street fentanyl, which put them at daily risk of death?
These questions are at the heart of drug policy and the way we view and treat addiction. But simplistic answers have stymied efforts to ameliorate drug use disorders and reduce stigma.
Research now shows that addiction doesn’t mean either being completely subject to irresistible impulses, or making totally free choices. Addiction’s effects on decision-making are complex. Understanding them can help policymakers, treatment providers and family members aid recovery.
Claims that people with addiction are unable to control themselves are belied by basic facts. Few of us inject drugs in front of the police, which means that most are capable of delaying use. Addicted people often make complicated plans over days and months to obtain drugs and hide use from others, again indicating purposeful activity. Those given the option will use clean needles. Moreover, small rewards for drug-free urine tests — used in a treatment called contingency management — are quite successful at helping people quit, which couldn’t be possible if addiction obliterated choice.
However, those who contend that substance use disorder is just a series of self-centered decisions face conflicting evidence, too. The most obvious is the persistence of addiction despite dire losses like being cut off by family members or friends, getting fired, becoming homeless, contracting infectious diseases or being repeatedly incarcerated.
Most people who try drugs don’t get addicted, even to opioids or methamphetamine, which suggests that factors other than simply being exposed to a drug can contribute to addiction. The majority of people who do get hooked have other psychiatric disorders, traumatic childhoods or both — only 7 percent report no history of mental illness. Nearly 75 percent of women with heroin addiction were sexually abused as children — and most people with any type of addiction have suffered at least one and often many forms of childhood trauma. This data implies that genetic and environmental vulnerabilities influence risk.
So how does addiction affect choice? Neuroscientists and philosophers are beginning to converge on answers, which could help make policy more humane and more effective.
Brains can be seen as prediction engines, constantly calculating what is most likely to happen next and whether it will be beneficial or harmful. As children grow up, their emotions and desires get calibrated to guide them toward what their brains predict will meet their social and physical needs. Ideally, as we develop, we gain more control and optimize the ability to choose.
But there are many ways that these varied processes can go awry in addiction and alter how a person makes choices and responds to consequences.
Traditionally, researchers focused on how the drug experience changes during addiction. At first, using is fun, perhaps exciting, perhaps soothing. It solves a problem like social anxiety or an absence of pleasure. Then, however, it becomes less effective: More is needed to get the desired effects, and coping without it begins to seem impossible. As addiction becomes ingrained, the craving for drugs intensifies even as they become less enjoyable.
In my own experience with cocaine, this disconnect was pronounced. At first, I found it euphoric. Toward the end of my addiction, I was injecting dozens of times a day, desperately wanting coke but also knowing it would make me feel hideous. The incentive salience theory suggests that addiction is a problem of outsized “wanting” despite reduced “liking,” which becomes less amenable to cognitive control over time.
During addiction, people also tend to prioritize short-term rewards over long-term gains, which means that they postpone the pain associated with quitting, often indefinitely. This idea, which is known as “delay discounting” further helps explain why people with chaotic childhoods and precarious incomes are at higher risk: When a better future seems unlikely, it is rational to get whatever joy you can in the present.
Chandra Sripada, professor of psychiatry and philosophy at the University of Michigan, argues that distorted thinking is more important in addictive behavior than overwhelming desire, leading to what he calls “unreliable” control over use. He focuses on how addiction affects our stream of consciousness.
During addiction, he contends, despairing thoughts about oneself and the future — not just thoughts about how good the drug is — predominate. At the same time, thoughts about negative consequences of use are minimized, as are those about alternative ways of coping. Drugs are overvalued as a way to mitigate distress; everything else is undervalued. The result is an unstable balance, which, more often than not, tips toward getting high.
This theory is helpful for explaining who is most likely to get addicted and what is most likely to generate recovery. Risk factors like poverty, a traumatic childhood and mental illness generate excess stress while tending to produce negative thoughts about oneself. In my case, I was depressed and isolated because of what I later learned was undiagnosed autism spectrum disorder — and hated myself for my inability to connect. The result was a mental climate conducive to relying on drugs, even when they no longer provided relief.
Factors linked to recovery — like social support and employment — can offset distorted thoughts and inflated valuation of drug use. Essentially, people make better choices when they recognize and have access to better options. If you are locked in a room with an escape route unknown to you hidden under the carpet, you are just as trapped as if that exit didn’t exist. My recovery began when I saw that there was a bearable way out.
This is why punitive approaches so often backfire: Causing more pain for people who view drugs as their only way to cope drives desire to use even more. Punishment doesn’t teach new skills that can allow better decisions. I was just lucky that I got help before it was too late.
But if addicted people are making choices that are harmful to themselves or others, shouldn’t they be held responsible for their behavior? Hanna Pickard, distinguished professor of philosophy and bioethics at Johns Hopkins University, calls for a framework she labels “responsibility without blame.” In this view, addicted people do have some control over their decisions. However, that doesn’t mean they deserve blame or that shaming and punishing them will improve matters.
Instead, providing people with both the skills and the resources they need to change, and compassionately holding them accountable as they learn to make different choices, can promote recovery. (This approach is a therapeutic one, not aimed at adjudicating addiction-related crimes, although the idea could potentially be extended into the legal realm.)
Research finds that framing addictive behavior as an involuntary brain disease reduces the tendency to blame people for it. But this perspective does not necessarily alleviate stigma or the desire to punish. This is probably because viewing individuals as having no autonomy dehumanizes them and makes others want to lock them up in an attempt to protect society.
The “responsibility without blame” concept offers a way around this: People with addiction have agency, but it is compromised. And this is not unique to addiction.
“I will have less control, if I’m exhausted and tired and upset, than if I’m well-slept in a stable happy place in my life,” said Professor Pickard, noting that being “hangry” is a classic example of diminished emotional control.
To recover, people with addiction need both new skills and an environment that provides better alternatives. This doesn’t mean rewarding people for bad behavior. Instead, we must recognize that compulsive drug use is far more often a response to a life where meaning and comfort appear out of reach than it is a selfish quest for excess pleasure.
April 2023 Neptune Alliance Prevention Article
Xylazine Is Deadly Drug Trend, Warns U.S. Government Agencies
Xylazine is a horse tranquilizer illicitly obtained and mixed with street opioids (such fentanyl and heroin) and “speed balls” (a combination of heroin and cocaine) to increase the user’s high. It also may be added to illicit drugs unbeknownst to the user to increase dealers’ profits.
The street supply of xylazine drug comes from veterinary use diversion and illicit manufacturing; officials are trying to determine how much of it comes from these routes. Xylazine is not FDA-approved for human use and therefore has a high human mortality rate. It is also not currently on the Drug Enforcement Administration’s (DEA’s) Schedule of Controlled Substances.
The side effects of xylazine include sleepiness, sedation, pain control, extreme muscle relaxation, low body temperature, low heart rate, low blood pressure, and decreased breathing, much like an opioid. However, since xylazine is not an opioid, its effects are not reversible with naloxone (Narcan), an opioid overdose antidote.
The more xylazine is used, the stronger its sedative effects will be, causing breathing and heart rate to slow down to sometimes fatal levels. It can also lead to skin abscesses and ulcers that may require eventual amputation.
Xylazine has become increasingly common across the U.S. in alarming quantities over the past several years. It was found in about 800 U.S. drug deaths in 2020, most of which occurred in the Northeast, and was detected in over 3,000 fatalities nationwide in 2021, according to the DEA in a 2022 report.
Learn more about xylazine here:
- Associated Press article: “An Emerging Threat: Drug Mix of Xylazine, Fentanyl”: https://apnews.com/article/veterinary-drug-fentanyl-xylazine-emerging-threat-a6bd800757575385fd878b4335f67c6d
- DEA publication: The Growing Threat of Xylazine and Its Mixture with Illicit Drugs: https://www.dea.gov/sites/default/files/2022-12/The%20Growing%20Threat%20of%20Xylazine%20and%20its%20Mixture%20with%20Illicit%20Drugs.pdf.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
How Can You Support the Mental Well-Being of Youth in Your Life?
Neptune Municipal Alliance March 2023 Prevention Article
Adriana Kuch died by suicide at 14 years old, days after classmates at her New Jersey high school in the Central Regional School District physically attacked her on February 1st. Video of the attack was posted online, calling attention to the very serious mental health, bullying, and violence issues our youth are facing today.
A recent Centers for Disease Control and Prevention study found that in 2021, almost 3 in 5 teenage girls felt persistent sadness in 2021—2 times the rate of boys and the highest rate of sadness reported in the past 10 years. The study also revealed that 1 in 3 girls and 22% of all students had seriously considered attempting suicide. Suicide is the second leading cause of death for U.S. adolescents and young adults.
Here are strategies adults can use to support the mental well-being
of youth they care about:
- If a child or teen you know is showing signs of substance use, anxiety, depression, suicide ideation, or another mental health challenge, it is critical to seek assistance right away. Listen non-judgmentally, show compassion, and enlist the expertise of professionals.
- When it comes to your own child or a child in your care, a good place to start is with their pediatrician or school student assistance coordinator/counselor (SAC), whose contact information can be found on their school’s website. You can also call your health insurer for a list of behavioral health professionals.
- Please share with your child or teen the 2ndFLOOR youth helpline (2/47, call or text): 888-222-2228. For those ages of 10 and 24, counselors at the helpline can offer support for issues large and small, from thoughts of self-harm to bullying and relationship issues with parents or peers. The 2ndFLOOR website also has comprehensive information on a variety of behavioral health issues: https://www.2ndfloor.org/.
- People of all ages can text “HOME” to 741741, the Crisis Text Line, for 24/7 support from a live, trained crisis counselor during any type of crisis.
- For substance use and mental health support for children and teens, families can reach out to the Family Crisis Intervention Unit (FCIU), 732-542-2444 day/ 732-996-7645 night and PerformCare, NJ Youth’s System of Care, 877-652-7624.
- Anyone experiencing suicidal thoughts or mental health-related distress can call or text 9-8-8, the Suicide and Crisis Lifeline, for 24/7, multi-lingual support.
- Remember to ALWAYS CALL 9-1-1 IN AN EMERGENCY!
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
“Prevention Starts with Parents” Toolkit
Please CLICK HERE to view

Struggling with Your New Year’s Resolution to Quit Smoking or Vaping?
Help to Follow Through Is Here!
February 2023 Neptune Alliance Prevention Article
When it comes to e-cigarettes, synthetic nicotine, nicotine salts, and no regulations for nicotine potency caps, today’s sources of nicotine are more powerful than ever, causing even stronger nicotine addiction and more intense withdrawal symptoms.
Many youth and adults think nicotine eases anxiety, depression, and stress, but taking in nicotine is actually just temporarily alleviating the withdrawal symptoms that nicotine addiction created in the first place, including anxiety, depression, and agitation.
Nicotine has a negative impact on mental health and intensifies anxiety and depression. Truth Initiative survey data shows support for the link between youth quitting nicotine use and improved mental health outcomes:
- 90% of youth survey respondents who quit vaping nicotine said they felt less stressed, anxious, or depressed;
- 47% of youth survey respondents who quit vaping reported that when they quit, they felt more in control;
- 78% of youth survey respondents who reported ever vaping but had not quit said they would feel better about themselves if they quit vaping (source: Truth Initiative’s article “How Quitting Nicotine Can Improve Mental Health,” https://truthinitiative.org/research-resources/quitting-smoking-vaping/how-quitting-nicotine-can-improve-mental-health?).
This Is Quitting (https://truthinitiative.org/thisisquitting) is the first-of-its-kind texting program to help youth, teens, and young adults quit vaping. It has become a free resource for 500,000+ young people. Access This Is Quitting by texting “DITCHVAPE” to 88709.
RWJ Barnabas Health’s free, 8-week Nicotine and Tobacco Recovery Program and its certified tobacco treatment specialists can help with the challenges associated with quitting. The program serves people of all ages and offers individual and group sessions, as well as nicotine replacement therapy (for those 18 and over).
To learn more about RWJ Barnabas Health’s Nicotine and Tobacco Recovery Program or to get started, visit https://www.rwjbh.org/treatment-care/institute-for-prevention-and-recovery/programs/nicotine-and-tobacco-recovery-program. For more information, watch RWJ Barnabas Health’s short video on quitting smoking: https://youtu.be/HHzJAMWbzmA.
Know that it is never too late…or too soon…to quit smoking and tobacco use! Read “Health Benefits of Quitting Smoking Over Time” on the American Cancer Society’s website: https://www.cancer.org/healthy/stay-away-from-tobacco/benefits-of-quitting-smoking-over-time.html.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse

Neptune Alliance, January 2023 Prevention Article
Inhalants Abuse
Inhalants are mostly used by children and teens, with about 20% of eighth graders reporting having used inhalants, according to a Drug Enforcement Administration (DEA) survey. Since they are legal to purchase and possess, easy to access, blend in with everyday items, and don’t cost a lot of money, inhalants are a popular substance for youth to abuse.
Inhalants contain chemical substances that have psychoactive, or mind-altering properties when inhaled through the nose or mouth. Within minutes of inhalation, the user experiences an intoxication similar to that of drinking too much alcohol: slurred speech, lack of coordination, euphoria, dizziness, and drowsiness.
Commonly abused inhalants include markers, glue, rubber cement, deodorant, hairspray, cleaning fluids, air fresheners, disinfectants, correction fluid, compressed air, spray paint, paint thinner, butane, gasoline, shoe polish, whipped cream in canisters, and cooking spray. The intoxication from an inhalant lasts just a few minutes, causing many users to inhale repeatedly for several hours. This can cause a loss of consciousness and/or death by asphyxiation. Some users will put cover their head in a plastic bag to inhale fumes.
While negative effects from short-term use of inhalants may be reversible, damage caused by long-term inhalants use is often permanent. Symptoms of prolonged use are muscle fatigue, confusion, inability to pay attention, irritability, excitability, depression, anxiety, weight loss, convulsions, and damage to the nervous system, heart, and other organs. There may also be trouble in school, such as absences and low grades.
Warning signs of inhalants abuse include paint or chemical stains on the hands or clothing, irritation around the mouth, red and watery eyes, a runny nose, a chemical odor on the breath, drunken behavior, disorientation, dizziness, loss of coordination, nausea, and a lack of appetite.
Learn more about inhalants abuse in the DEA’s “Inhalants” fact sheet: https://www.dea.gov/sites/default/files/2020-06/Inhalants-2020_1.pdf.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Neptune Alliance December 2022 Prevention Article
December Is Drugged and Drunk Driving Prevention Month!
Remember, Holiday DUI Deaths Are 100% Preventable!
In 2019, during the week between Christmas and New Year’s Day, 210 people died in alcohol-impaired driving crashes, according to the National Highway Safety Traffic Administration (https://www.samhsa.gov/blog/national-impaired-driving-prevention-month).
Over 26 million people ages 16 and older drove under the influence or alcohol and/or illicit drugs during 2019, and 17% of these drivers were 20 to 25 years old, states the U.S. Department of Health’s SAMHSA 2020 National Survey on Drug Use and Health (https://www.samhsa.gov/blog/national-impaired-driving-prevention-month).
Since recreational marijuana was legalized in Colorado in 2013, Rocky Mountain High Intensity Drug Trafficking Area data reports that traffic deaths in which drivers tested positive for marijuana increased 135%, while all Colorado traffic deaths increased 24%. This equates to one person killed every 3.5 days in 2019 compared to one person killed every 6.5 days in 2013 (https://www.thenmi.org/wp-content/uploads/2020/10/RMHIDTA-Marijuana-Report-2020-2.pdf).
In addition to alcohol, many substances can lead to driving under the influence (DUI), including marijuana, opioids, methamphetamines, stimulants, and even prescribed and over-the-counter medications. Remember, if you feel different, you drive different! It is illegal and potentially deadly to drive under the influence of any substance.
Here are a few life-saving pointer to remember this holiday season—and all year round—when it comes to preventing a DUI tragedy:
- Before drinking or taking any impairing drug, plan a safe and sober ride home ahead of time through a family member/friend, ride share service, or public transportation
- Don’t let someone get behind the wheel if they are impaired by any substance; take the keys!
- If you’re hosting a gathering, make sure all guests have a sober ride home, or let them stay put
- If you see an impaired driver, call 911
- Always wear your seat belt–it’s your best defense against impaired drivers
If you or someone you know struggles to stop drinking or using a substance despite the negative impacts and dangers it may cause, help resources are available. The Substance Abuse and Mental Health Services Administration (SAMHSA) National Helpline, 1-800-662-HELP (4357) is a confidential, free information service, available 24/7 in English and Spanish. The SAMHSA National Helpline assists individuals and family members facing mental and/or substance use disorders by providing referrals to local treatment facilities, support groups, and community-based organizations. Learn more about the helpline here: https://www.samhsa.gov/find-help/national-helpline.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Neptune Alliance, November 2022 Prevention Article
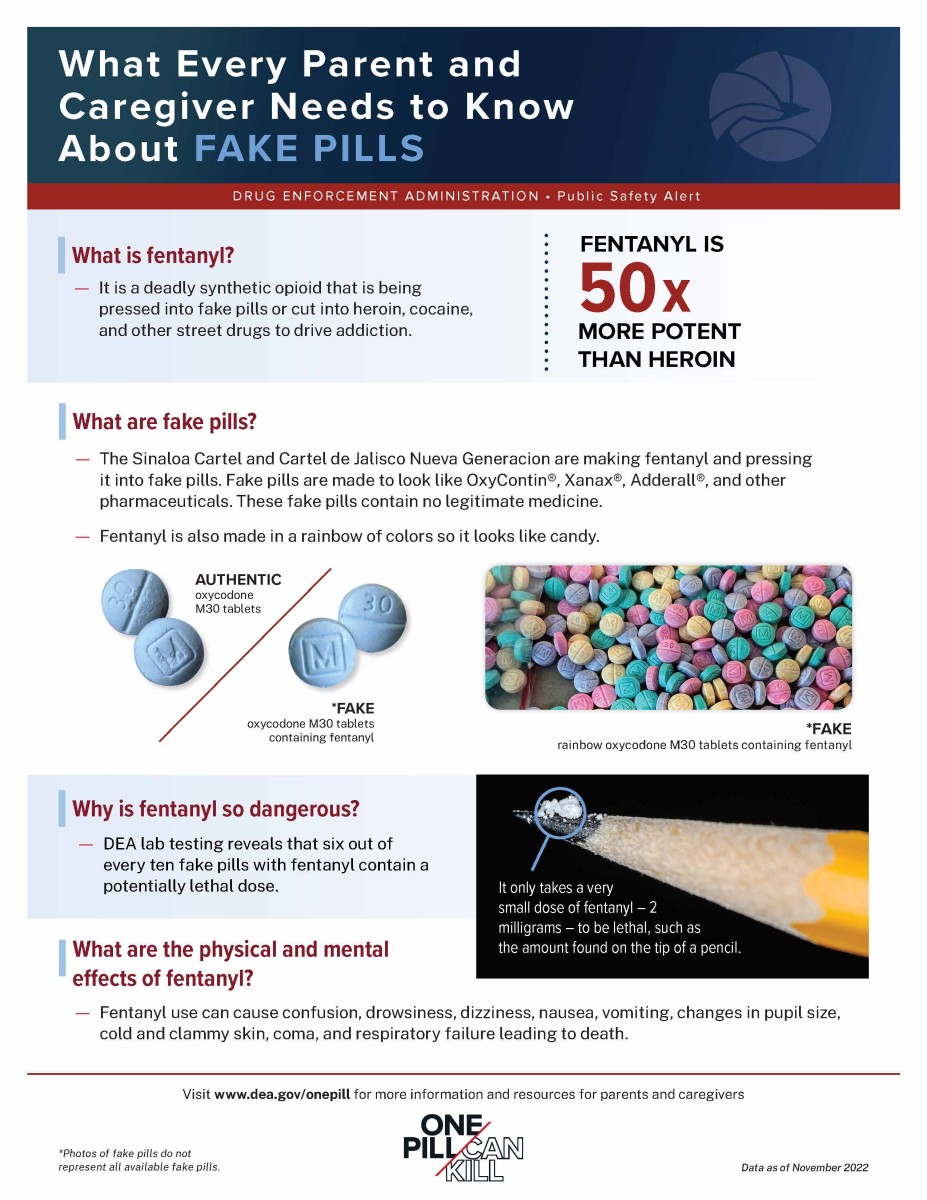
“One Pill Can Kill!” the DEA Warns People of All Ages
The U.S. Drug Enforcement Administration’s (DEA) “One Pill Can Kill” campaign warns how criminal drug networks are mass-producing counterfeit pills and falsely marketing them as legitimate prescription pills.
The fake pills are made to look like pharmaceutical drugs such as Percocet®, Xanax®, Adderall®, Vicodin®, and OxyContin®. It can be nearly impossible to tell the difference between illicit and real prescription pills. Drug cartels are also targeting youth on social media with counterfeit rainbow-colored pressed pills that resemble brightly colored candy, right down to their deceptive packaging.
Counterfeit pills are widely available and easy to purchase. They often contain fentanyl or methamphetamine and can be deadly. Fentanyl and other synthetic opioids account for about two-thirds of our nation’s 100,306 fatal overdoses between April 2020 and April 2021—the highest overdose rate ever reported for one year in the U.S. Deaths from methamphetamine and other psychostimulants increased almost 50% during this same time period.
Fentanyl is 50-times more potent than heroin. Just 2 milligrams of fentanyl—an amount that fits onto a pencil point—can be deadly. The DEA estimates that 4 out of every 10 counterfeit pills that contain fentanyl have a deadly dose. A rainbow fentanyl bust in New York this fall found 15,000 illicit pills hidden in Legos—enough fentanyl to kill 500,000 people.
Early education to build awareness is key, and the DEA urges parents to have age-appropriate conversations with their children as young as the elementary school grades to be aware of what they are consuming and to make healthy choices. People of all ages should only take drugs that are prescribed by their doctor specifically for them and filled by their pharmacy.
Learn more about the DEA’s “One Pill Can Kill” campaign at https://www.dea.gov/onepill. The fact sheet also provides side-by-side comparisons of legitimate versus fake pills.
Adults caring for youth should read the DEA’s public safety alert “What Every Parent and Caregiver Needs to Know About Fake Pills”: https://www.dea.gov/sites/default/files/2022-09/DEA-OPCK_Parent%20flyer.pdf.
“Emoji Drug Code—Decoded” is another great DEA resource for parents, caregivers, educators, and other influencers to learn how emojis are being used in conjunction with illegal drugs: https://www.dea.gov/sites/default/files/2021-12/Emoji%20Decoded.pdf.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Neptune Alliance, October 2022 Prevention Article
October Is National Bullying Prevention Month!
Bullying is unwanted, aggressive behavior among school aged children that involves a real or perceived power imbalance. The behavior is repeated, or has the potential to be repeated, over time. Both kids who are bullied and who bully others may have serious, lasting problems. Bullying can be verbal, social, and/or physical.
Cyberbullying is bullying that takes place over digital devices like cell phones, computers, and tablets.
According to Pacer’s National Bullying Prevention Center’s statistics, one out of every 5 students in America reports being bullied, almost 50% of tweens (ages 9 to 12 years old) report experiencing bullying at school, and 14.5% of tweens report experiencing cyberbullying (https://www.pacer.org/bullying/info/stats.asp).
Students who experience bullying are at increased risk for depression, anxiety, lower self-esteem, sleep difficulties, physical ailments, lower academic achievement, dropping out of school, and relationship difficulties
StopBullying.gov (https://www.stopbullying.gov/) provides information on what bullying is, what cyberbullying is, who is at risk, how you can prevent and respond to bullying, and bullying support resources.
October Is National Substance Abuse Prevention Month!
Millions of Americans suffer from substance abuse–including underage drinking and marijuana use, alcohol misuse, abuse of prescription and over-the-counter medications, and street drugs.
Over 100,000 overdose deaths occurred between April 2020 and April 2021–the highest number ever recorded in the U.S. in one year. Over 80,000 of these deaths were due to opioid overdoses—mostly illegally manufactured fentanyl mixed with other illicit drugs.
Any form or substance use—including nicotine, marijuana, alcohol, illicit drugs, synthetic drugs, and prescription medications—can permanently impact youth’s brain development, with the brain developing until at least age 25. Youth and young adult substance use increases the lifetime risk of developing a substance use disorder, a long-term mental health disorder, poor physical health, lowered career and financial achievement, and negative social consequences
Immediate and proper disposal of unused, unwanted prescription and over-the-counter medications prevents ease of access to medications and medication abuse by family members, guests, and teens, which can lead to addiction.
For information on safe medication disposal, visit the U.S. Food and Drug Administration’s “Where and How to Dispose of Unused Medications”: https://www.fda.gov/consumers/consumer-updates/where-and-how-dispose-unused-medicines.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
September 2022 Neptune Alliance Prevention Article
September Is National Suicide Prevention Month

With post-pandemic rises in anxiety, depression, suicide ideation, and substance use across all ages, September Is National Suicide Prevention Month focuses on creating awareness of suicide prevention, mental health support resources, and crisis helplines.
In 2020, 45,979 Americans died by suicide and 1.2 million Americans attempted suicide, according to the Centers for Disease Control and Prevention’s most recent statistics. Suicide is the 2nd leading cause of death for 20- to 34-year-olds and the 3rd leading cause of death for 10- to 19-year-olds in the U.S.
With suicide and mental health/substance use disorders, immediate intervention and professional assistance save lives, as does knowing, recognizing, responding to, and taking seriously the warning signs of suicide.
The warning signs of suicide include…
- talking about dying or death
- feeling hopeless with no reason to live
- having a suicide plan
- expressing great shame
- feeling trapped without solutions
- sharing about unbearable pain
- using alcohol or drugs more often
- changing daily behavior and grooming habits
- giving away special possessions
- withdrawing from family and friends.
Mental Health First Aid and Question, Persuade, Refer (QPR) trainings, whether completed virtually or in person, provide simple steps anyone can learn to help save a life from suicide. Just as people trained in CPR help save thousands of lives each year, people trained in Mental Health First Aid or QPR learn how to recognize the warning signs of a suicide or mental health crisis and how to implement strategies to effectively assist someone with getting the help they need. For more information, visit the Mental Health First Aid website at https://www.mentalhealthfirstaid.org/ and the QPR website at https://qprinstitute.com/.
It is also important to be familiar with suicide prevention resources to use and share:
- 9-1-1 should always be called in an immediate crisis, emergency, or dangerous situation
- National Suicide, Mental Health and Substance Use Crisis Lifeline (24/7, talk/text): 9-8-8, https://988lifeline.org/
- NJ Hopeline (24/7): 855-654-6735, http://www.njhopeline.com/
- 2ndFLOOR Youth Helpline (24/7, talk/text): 888-222-2228, https://www.2ndfloor.org/
- Crisis Text Line (24/7): Text “Home” to 741741, https://www.crisistextline.org/
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
Neptune Alliance, July 2022 Prevention Article
Universal Hand Signal for Help
The “Signal for Help,” also known as the “Violence at Home Signal for Help,” is a universal hand gesture for abuse victims to discreetly reach out for assistance, either remotely during a video chat or call or while in public. The hand signal is a reminder of the power of situational awareness, looking out for each other, and stepping up to help someone during a time of distress.
Folding the thumb across the palm and then closing the remaining 4 fingers down over it is an internationally recognized sign for help due to violence at home or another life-threatening situation. Someone in distress can use the Signal for Help to quietly summons assistance, without the risk of their perpetrator overhearing or finding a digital trace online. The motion can be done over and over again, rather than a single motion held in position that may not be as readily observed.
If someone motions with the Signal for Help in a video chat or call, contact the person using another means of communication (a text, cell phone call, or email) and ask simple yes or no questions so they can respond without tipping off their perpetrator who may be present and listening. Call the police only if the signaler directly asks you to, as it can escalate the situation.
The Canadian Women’s Foundation created the Signal for Help in April 2020 in response to increased domestic violence during the COVID-19 pandemic’s social isolation and distancing, when someone may have been forced into isolation with their perpetrator with just brief occasions for remote social contact via video applications.
A female teenager in Kentucky used the Signal for Help through the car window to alert her distress to a motorist driving alongside her vehicle, who immediately called the police for help. Watch this video on how the hand gesture saved the young woman’s life: https://youtu.be/oU3jZT3b9Uc.
For more about the Signal for Help, watch this video: https://youtu.be/AFLZEQFIm7k.
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse
17th Annual NEPTUNE TOWNSHIP COPS VS. KIDS Game
The Neptune Township Municipal Alliance to Prevent Substance Misuse would like to extend a huge thank you to all who helped make the seventeenth annual Cops vs. Kids game such a success!
It was a great event—from pre-event sponsorship to the last out. The Cops played the kids in a whiffle ball game on June 6 at Neptune High School. The weather was gorgeous, the verbal taunts were flying, and the game was a hoot, with the Cops and Kids enjoying some friendly competition!
Spectators got to join in the fun, and there were prizes for all the kids!
Thanks to Jim MacConchie for organizing the Cops, and to Catherine Crelin for assembling the Kids.
Thanks also to event sponsors, including: Neptune Police PBA #74, Neptune FOP #19, Jersey Mike’s Subs, Theo’s Demolition & Construction Clean-Up, Impact Auto Body, Bruno’s Italian Deli, MJ’s Restaurant Bar & Grill, McDonalds, Allied Fire & Safety, Uni-Serv, MURC, Neptune Board of Education & High School, the Neptune Municipal Alliance to Prevent Substance Misuse, and the Neptune Recreation Department. Funding for this event is also provided through the Governor’s Council on Alcohol & Drug Abuse.
Thanks to everyone who supported the game, and in turn, helps us spread our prevention message to the community. Be sure to look for our next Cops vs. Kids fundraiser, as I heard there’s a re-match coming!
Sincerely,
Dawn Thompson, Recreation Director &Coordinator, Municipal Alliance to Prevent Alcoholism and Drug Abuse



Neptune Township’s ‘Hooked on Fishing’ Event a Huge Catch
The sky was bright, with barely a cloud in the sky, and the pond packed with fish this past Sunday in Neptune, as over 110 youth tried their luck at this year’s 6th annual ‘Hooked on Fishing, Not on Drugs’ event. The free tournament was held at the Hamilton Fire Company Pond and organized by the Neptune Township Municipal Alliance to Prevent Substance Misuse, Recreation, Police, and Marina; Bradley Beach Surf Casters; and Ocean Grove Fishing Club.
The fish were biting early, as kids went running to measuring stations all around the pond, operated by volunteers from the Surf Casters and Fishing Club, with fresh-caught bass, catfish, bluegills and sunnies. Everyone was smiling and enjoying the great outdoors as shouts of “I got one!” were heard around the pond with each new catch. Prizes and trophies for biggest catch, provided by the two fishing clubs, were awarded to Skyler W (18oz, 14” catch) in the 1-6 age group, Gavin K. (24.5oz, 13.75” catch) in the 7-10 age group, Marissa P (37oz, 17.5” catch) in the 11-14 age group, and Logan B. (10oz, 11” catch) in the 15-18 age group. Over a dozen other prizes were awarded throughout the event!
For use of the pond, hats, towels, bait, and trophies, special thanks to event sponsors—Hamilton Fire Company, Imperial Healthcare, Seacrest Recovery, Dick’s Sporting Goods, the Governor’s Council on Alcoholism & Drug Abuse, Mike’s Pet Supply, Jody & Jodee’s Fishery, Tony’s Pizza, and The Cone Zone. It was a perfect day for fishing! There were even special appearances made by Mr. Turtle and Ms. Snake!
NJ Department of Environmental Protection designed the Hooked on Fishing Not on Drugs event to create an interest in safe, healthy, outdoor activities for youth, and Neptune Township is proud to be an event supporter. Look for our 7th annual Hooked on Fishing event next year!!


Neptune Alliance, June 2022 Prevention Article
When Gambling Becomes a Problem
Gambling addiction, compulsive gambling, and problem gambling can happen to anyone. It is when occasional gambling for fun and entertainment becomes an obsessive behavior with serious consequences.
Whether a person bets on professional or college sports, races, scratch-offs, or card or casino games, a gambling problem can strain relationships, interfere with work, and lead to financial disaster that leads to running up huge debts or stealing money. Problem gambling can occur with placing bets online and through apps, as well as with betting in person at casinos and tracks.
With compulsive gambling, a person can’t control the urge to gamble, even when it has negative consequences for themselves or loved ones. Problem gambling is any gambling behavior that disrupts a person’s life. If someone is preoccupied with gambling, spending more and more time and money on it, trying to recuperate from losses, or continuing to gamble despite serious life consequences, they have a gambling problem. Gambling addiction is often accompanied by stress, anxiety, and substance use and mental health disorders.
Overcoming gambling problems starts with acknowledging that you have a problem. Self-help strategies to stop gambling addiction include identifying underlying reasons why you gamble, such as certain situations, behaviors, or emotions that act as triggers; building a supportive network of friends, family, and colleagues who do not engage in gambling; shifting your activities to include new hobbies, sports, or exercise; making meditation and other relaxation practices part of your daily routine; joining support groups like Gamblers Anonymous (see the information below); and seeking professional assistance for underlying mental health issues.
If you or someone you care about may have a gambling problem, the National Council on Problem Gambling Helpline is a confidential, 24/7 helpline for problem gamblers or their family members (800-522-4700 or https://www.ncpgambling.org/).
There is also support available through the Gamblers Anonymous 12-step program (855-222-5542 or https://www.gamblersanonymous.org/ga/).
Article by Christa Riddle, All About Writing
Brought to you by the Neptune Municipal Alliance to Prevent Substance Misuse and the Governor’s Council on Alcoholism & Drug Abuse

Monmouth County
2021-22 Children & Youth
Behavioral Health
Resource Guide
Please CLICK HERE to view this guide
Vaping Disease EVALI Called Attention to E-Cigarette Risks

- 2,800+ cases of e-cigarette, or vaping, product use associated lung injury (EVALI) hospitalizations were reported in the U.S. and its territories
- 68 EVALI deaths were reported across 29 states and Washington D.C.
- The median age of patients who died from EVALI was 49.5 years, with an age range from 15 to 75 years (above numbers reported as of 2-18-2020)
Vaping products with THC proved to be prevalent in the reported cases of e-cigarette, or vaping, product use associated lung injury (EVALI). THC was found in most of the tested products, and most patients reported a history of using products containing THC—THC (tetrahydrocannabinol) is the psychoactive component of marijuana that produces the high sensation. Vitamin E acetate was found in FDA- and state-lab-tested product samples, as well as nationwide CDC-tested patient lung fluid samples.
Affected EVALI patients presented a variety of symptoms, including coughing, pleuritic chest pain, shortness of breath, fatigue, fever, chills, headaches, nausea, vomiting, appetite loss, and diarrhea. Patients were hospitalized due to a need for respiratory support and ventilation, and all had a history of vaping.
As an immediate response to the initial EVALI outbreak in 2019, The Centers for Disease Control and Prevention (CDC) recommended avoiding use of all e-cigarette and vaping products to eliminate risk. They later amended risk control as refraining from using e-cigarettes specifically containing THC, and that Vitamin E acetate should not be added to e-cigarette or vaping products.
In general, the CDC states that e-cigarette or vaping products with nicotine or THC should never be used by youths, young adults, and pregnant women, and that adults who do not currently use tobacco products should not start using these products.
Vaping Risks Beyond EVALI
The alarming rise of youth vaping has been, in part, fueled by a lack of parent and youth education regarding the risks surrounding e-cigarettes, before and after the EVALI outbreak. Because vapes resemble familiar school supplies such as pens and flash drives, are easy to conceal, and do not emit the tell-tale odors of traditional cigarettes or marijuana joints, young people are vaping in school, right in the company of their teachers.
After inhaling the vapor, teens exhale into water bottles or their shirts to avoid detection. Adding to the youth vaping epidemic is the fact that the sleek devices and their appealing flavors are marketed in ways that attract teens.
Many youth and adults are unaware of the high nicotine potency delivered by e-cigarettes and refillable vaping devices that allow for customizable nicotine levels that are not regulated. A single Juul-manufactured pod houses the same amount of nicotine as a pack of traditional cigarettes; some youth smoke multiple pods in a day, spiking nicotine addiction that is difficult to stop and can lead to smoking traditional cigarettes. Many teens also vape THC.
Beyond nicotine, e-cigarette “juices,” or liquids, and their vapors contain a host of harmful and unregulated chemicals, including diacetyl, formaldehyde, heavy metals, oils, and volatile organic compounds that can cause permanent lung damage and cancer. Furthermore, the lungs are not inherently equipped to inhale vaporized liquids.
While it is illegal to sell smoking products, including e-cigarettes and vaping devices, to minors under the age of 21 in New Jersey, it is not illegal for youth under 21 to possess them, which is why parental education and a zero-tolerance for youth e-cigarette use is a necessary component in battling the youth vaping epidemic.
For more information on the dangerous realities of vaping, teens can visit the U.S. Surgeon General’s website “Know the Risks: E-Cigarettes and Young People” at https://e-cigarettes.surgeongeneral.gov/, as well as the interactive website “Behind the Haze” at https://www.behindthehaze.com/.
For the critical parent education component necessary to help halt this epidemic and its potential for permanent harm to youth, parents can visit Partnership for Drug-Free Kids’ “How to Talk to Your Kids About Vaping” (https://drugfree.org/article/how-to-talk-with-your-kids-about-vaping/). Their website also reports the latest news on e-cigarettes and vaping (https://drugfree.org/learn/drug-and-alcohol-news-tag/e-cigarettes-and-vaping/).
Smokefree.gov (https://teen.smokefree.gov/) provides resources for targeted audiences, including teens, on how to quit using electronic and traditional cigarettes.
RWJBarnabas Health Institute for Prevention and Recovery (https://www.rwjbh.org/treatment-care/mental-health-and-behavioral-health/mental-health-services/institute-for-prevention-and-recovery/programs/nicotine-and-tobacco-recovery-program/) offers a free nicotine and tobacco cessation program for people of all ages to help with quitting electronic and traditional cigarette use.
Is Youth Substance Use Really Influenced by
Parenting, Social Status & Environment?

“Does Socioeconomic Advantage Lessen the Risk of Adolescent Substance Use?” examines the influence parenting, socioeconomic status, and home and school environments have on adolescent substance use (socioeconomic status measures sociological/economic position—or class standing—based on education, income, and occupation).
The information in the article comes from new and on-going studies that shed light on how environmental risk/protective factors play a part in youth alcohol, drug, and tobacco use.
The studies presented in the article found…
- Excessive drinking by adolescents is associated with upper-middle-class families and parents who have college degrees and higher incomes
- Youth marijuana use is more closely associated with its acceptance in the school environment, rather than education or income
- Youth smoking is associated with socioeconomic disadvantage and less parental education
- Teen drug/alcohol use is highly predictive of adulthood problems like substance use disorders and is not necessarily outgrown
- Parental “zero tolerance” rules, open communication, and involvement play key roles in lessening or delaying adolescent substance use risk
- “Harm-reducing” parental rules aimed at only limiting excessive drinking yielded 150% higher youth alcohol consumption than “zero tolerance” parental rules
An Arizona State University study that followed two groups of students from affluent northeastern suburbs for 10 years (high school to adulthood) identified concerning rates of later substance use in the population who used drugs and alcohol during adolescence. Little evidence was found to indicate that the subjects matured out of substance use.
This same study revealed a rate of non-medical use of prescription stimulants double that of national norms, presented the likelihood of substance use disorder diagnoses that were two to three times above the national average, and showed strict parental rules against substance use delivered in a supportive, nurturing household were a strong protective factor against underage drinking and marijuana use.
Another study based on national adolescent-to-adult health data indicated school-age marijuana use as a significant predictor of use 14 years later. Young adults with more-educated parents were more likely to have used marijuana recently than those with less-educated parents.
While no group is immune from substance use or substance use disorders, different youth are at risk for different reasons, such as higher availability in disadvantaged environments and achievement and popularity pressures coupled with more disposable income in wealthier suburban areas. Affluent parents may also worry less about substance use because they see their children as committed to achieving success— and as youth who would never engage in substance use.
“Does Socioeconomic Advantage lessen the Risk of Adolescent Substance Use?” can be read in detail at https://www.hazeldenbettyford.org/education/bcr/addiction-research/socioeconomic-advantage-edt-818.

The Neptune Township Municipal Alliance to Prevent Alcoholism & Drug Abuse is working on a new 5-year plan to incorporate community–wide strategies to combat substance abuse. Join us in the cause to build a healthier, safer community—your ideas and support are welcome & needed.
Municipal Alliance
Dawn Thompson, Alliance Coordinator
dthompson@neptunetownship.org
732-869-1202







